In recent pharmacovigilance inspections, between 25–35% of major observations were linked to weak or inconsistent causality assessment in pharmacovigilance, particularly where safety conclusions could not be clearly defended during regulatory review. These findings highlight a recurring challenge for safety organizations: regulators increasingly expect causality decisions to demonstrate structured scientific reasoning, traceable data use, and consistent governance across reporting systems, in line with evolving expectations within Pharmacovigilance oversight.
This article explains how inspectors evaluate causality practices during inspections, why poorly supported causality conclusions frequently trigger repeat findings, and how inspection-ready pharmacovigilance teams design processes that withstand regulatory scrutiny.
Table of Contents
What Causality Assessment Means in Pharmacovigilance
Causality assessment is the structured evaluation of whether a medicinal product is reasonably related to an adverse event and forms a core decision-making element within causality assessment in pharmacovigilance.
From a regulatory perspective, causality assessment is not a subjective clinical opinion. Instead, it is a defined decision-making process that integrates case data, temporal relationships, biological plausibility, and existing safety knowledge to support consistent conclusions across individual case safety reports and aggregate reviews.
This process determines whether the available evidence supports a relationship between a medicinal product and an adverse event within a regulated safety framework. Inspectors therefore focus on how consistently causality decisions are applied across cases, products, and reporting timelines. Reliable assessment depends on methodical reasoning, documented justification, and alignment with established safety governance rather than isolated expert judgment.
Why Causality Decisions Influence Inspection Outcomes
Causality decisions influence inspection outcomes because regulators treat them as indicators of safety governance maturity, particularly when reviewing how causality assessment in pharmacovigilance supports consistent and defensible safety oversight.
During inspections, authorities examine whether causality conclusions support downstream activities such as signal detection, benefit–risk evaluation, and regulatory reporting. Inconsistent or weakly justified causality assessments raise concerns about an organization’s ability to control safety risks proactively.
Inspection experience shows that sites with robust causality frameworks resolve safety questions more efficiently, while those relying on ad hoc judgment face escalated findings when decisions cannot be defended across reviewers or over time.
How Inspectors Review Causality Assessment Practices
Regulators assess causality assessment through a structured review of how data, medical reasoning, and quality oversight function together during routine pharmacovigilance operations.
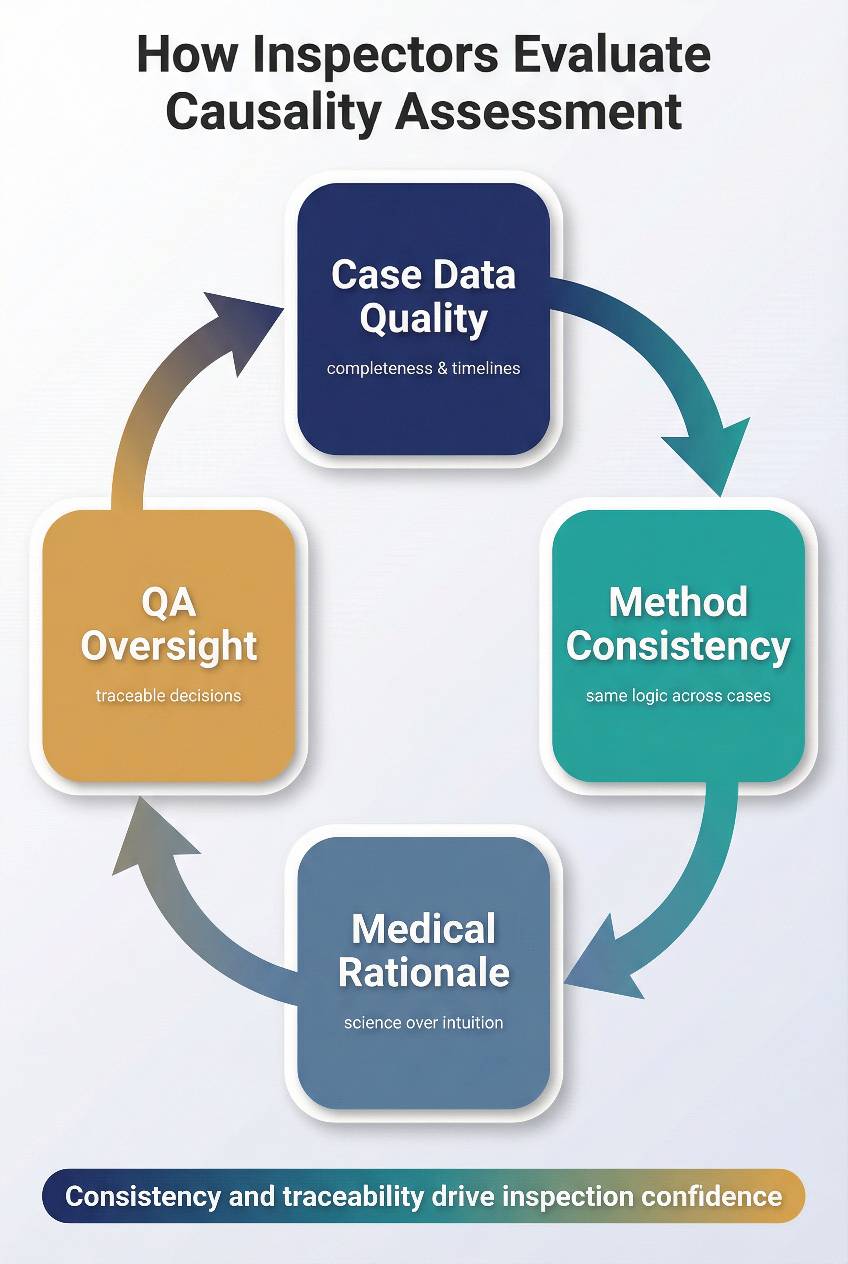
Inspectors review causality assessment practices by examining how data quality, scientific reasoning, methodological consistency, and quality oversight combine to support defensible safety decisions. Rather than judging individual case conclusions in isolation, they evaluate whether causality assessments remain coherent across cases, reviewers, and time especially when decisions influence signal management, regulatory reporting, or benefit–risk evaluation.
This review typically focuses on the following assessment areas:
- Data Completeness and Case Documentation Quality
- Consistency of Causality Methods Across Cases
- Medical Judgment and Scientific Rationale
- Traceability of Decisions and QA Oversight
Data Completeness and Case Documentation Quality
Data completeness forms the foundation of causality assessment. Inspectors assess whether individual case safety reports contain sufficient clinical detail, exposure information, timelines, and outcome data to support a reasoned conclusion.
In practice, inspection findings often arise when missing or inconsistent case data forces assessors to rely on assumptions rather than evidence, weakening the credibility of causality decisions.
Consistency of Causality Methods Across Cases
Consistency matters as much as methodology. Inspectors review whether the same causality approach is applied across similar cases, products, and reporting periods.
When different assessors reach divergent conclusions using identical data, regulators question whether the causality process is controlled or dependent on individual interpretation.
Medical Judgment and Scientific Rationale
Medical judgment remains essential, but inspectors expect it to be grounded in transparent scientific rationale. Causality conclusions should reference plausible mechanisms, known class effects, and supporting literature where relevant.
Micro-credibility insight: During inspections, regulators frequently challenge causality rationales that rely solely on clinical intuition without documented scientific support.
Traceability of Decisions and QA Oversight
Traceability ensures that causality decisions can be reviewed, reproduced, and defended. Inspectors assess whether assessments are documented clearly, reviewed appropriately, and subject to quality oversight.
Weak QA involvement often leads to inspection findings when causality decisions change without documented justification or escalation.
Where Causality Assessments Fail Under Regulatory Review
Regulatory review consistently reveals patterns of failure in causality assessment practices.
Common findings include incomplete case documentation, inconsistent application of assessment criteria, and insufficient linkage between individual case conclusions and aggregate safety evaluations. Inspectors also note gaps where causality decisions are not revisited when new data emerges.
These weaknesses undermine confidence in signal detection and benefit–risk evaluation, leading regulators to question the robustness of the overall pharmacovigilance system.
Building Inspection-Ready Causality Assessment Processes
Inspection-ready causality assessment follows a clear pathway that connects individual case data to defensible regulatory decisions through structured review and governance.
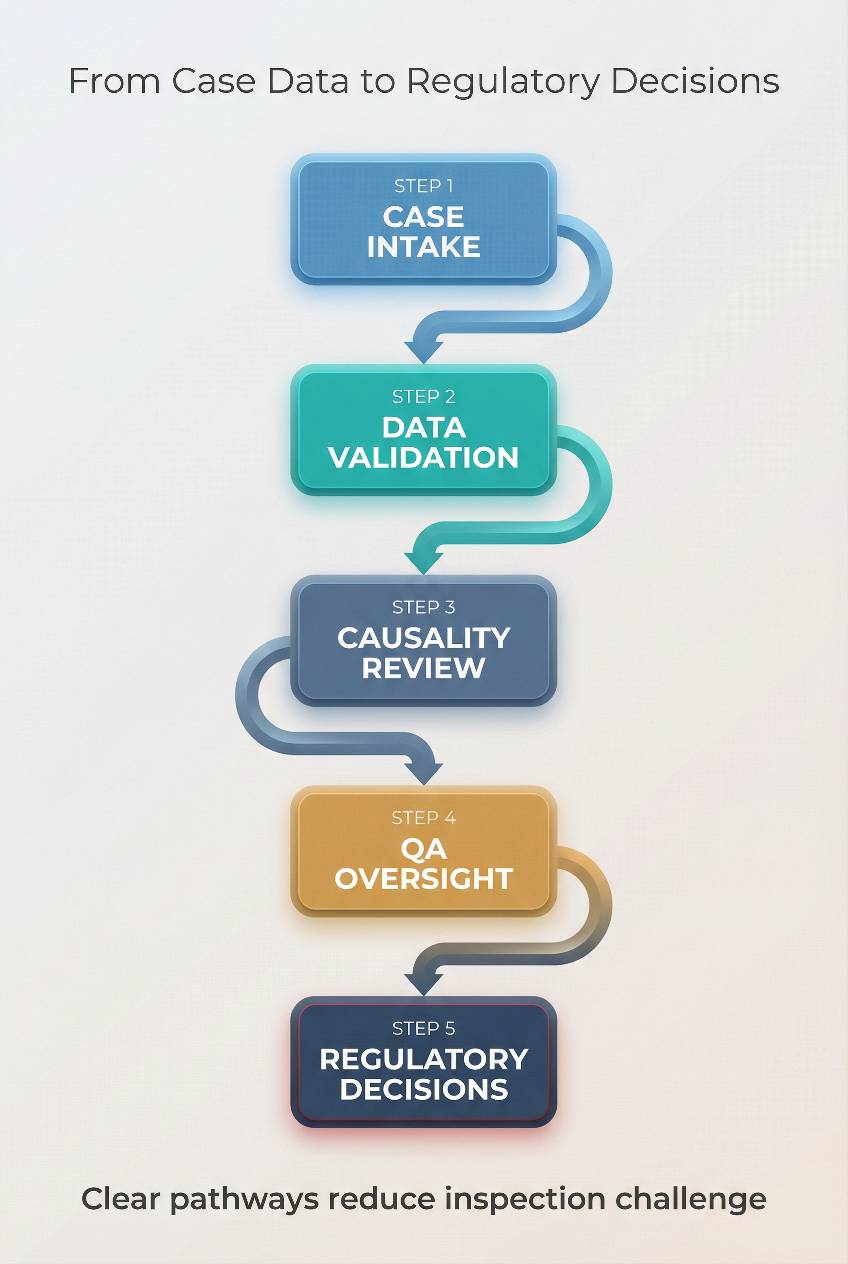
Effective improvements include:
- Standardizing causality methodologies across products and teams
- Strengthening data quality controls at case intake
- Embedding scientific rationale requirements into assessment templates
- Ensuring QA oversight of causality decisions and changes
- Linking individual case assessments to signal management workflows
Organizations that implement these measures demonstrate greater control during inspections and reduce the likelihood of repeat observations related to safety decision-making.
Final Word
Across recent regulatory inspections, approximately 20–30% of pharmacovigilance-related repeat findings were attributed to deficiencies in causality documentation and justification, particularly where earlier conclusions could not be defended during follow-up reviews. These outcomes reinforce a clear regulatory expectation: causality assessment in pharmacovigilance must function as a controlled, transparent process that supports signal evaluation and benefit–risk oversight, not as an isolated clinical exercise.
Teams that invest in consistent methods, strong data integrity, and clear governance reduce inspection risk, protect regulatory timelines, and strengthen confidence in safety decisions. In many cases, early warning signs of weak causality control appear long before inspectors formally raise concerns.
Micro-credibility insight: Inspection escalations often follow repeated internal disagreements on causality that were never formally resolved or documented.
FAQs
Inspectors look for complete case data, consistent assessment methods, and clearly documented scientific rationale that supports causality conclusions across similar cases and reporting periods.
Challenges arise when causality decisions rely on incomplete data, vary between assessors, or lack traceable justification linking individual cases to signal and benefit–risk evaluation.
Standardizing assessment templates, improving data completeness at case intake, and applying quality oversight to causality decisions improve inspection readiness without adding operational burden.

Mahtab Shardi
Mahtab is a pharmaceutical professional with a Master’s degree in Physical Chemistry and over five years of experience in laboratory and QC roles. Mahtab contributes reliable, well-structured pharmaceutical content to Pharmuni, helping turn complex scientific topics into clear, practical insights for industry professionals and students.

Pharma Jobs in Sydney in 2026: Salary, GMP and Hiring Trends
Sydney’s pharmaceutical sector continues to expand under strict TGA GMP inspection trends and PIC/S compliance Australia alignment. This article analyzes regulatory hiring growth, salary positioning, and compliance-driven career opportunities across manufacturing, quality assurance, and regulatory functions.

Quality Control (QC) in Pharma Industry: Top Strategies, Tests & Insights in 2026
Quality Control (QC) in the pharmaceutical industry is a vital process that ensures medicines meet stringent safety and quality standards. By detecting defects and contamination early, QC protects patients and supports regulatory compliance worldwide. Implementing strong QC systems safeguards the integrity and trustworthiness of pharmaceutical products.

Pharma Jobs in Melbourne in 2026: GMP Inspection and Salary Trends
Melbourne’s pharmaceutical sector continues to expand under strict TGA oversight. This analysis explores pharmaceutical manufacturing jobs Victoria, GMP inspection trends, salary benchmarks, and regulatory qualification pathways shaping compliance-driven career growth across sterile and biotech operations.